Knee Pain Management: Causes, Symptoms, and Treatment Options
Knee pain is a prevalent orthopedic concern that affects a significant number of individuals worldwide. The knee joint plays a crucial role in supporting our body weight and facilitating various movements, making it susceptible to injuries and degenerative conditions. Knee pain can arise from various causes, including sports injuries, overuse, arthritis, ligament tears, and fractures.
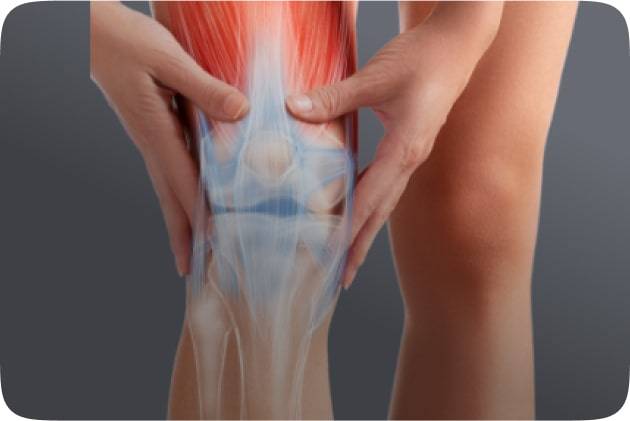
The knee joint is one of the largest and most complex joints in the human body, facilitating essential functions like walking, running, and jumping. It is a hinge joint formed by the articulation of three bones: the femur (thigh bone), tibia (shinbone), and patella (kneecap). These bones are held together by a network of ligaments, including the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL), which provide stability and prevent excessive movement.
Causes of Knee Pain
Osteoarthritis: Osteoarthritis is a degenerative joint disease that commonly causes knee pain. It occurs when the protective cartilage covering the ends of the bones in the knee joint gradually wears down over time. Risk factors for osteoarthritis include aging, previous knee injuries, obesity, repetitive stress on the joint, and genetic predisposition. Symptoms of knee osteoarthritis include pain, stiffness, swelling, decreased range of motion, and a grinding sensation during movement.
Ligament Injuries: The knee has four major ligaments, and injuries to these ligaments can cause significant knee pain. The anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) are often injured during sports or activities involving sudden stops, changes in direction, or direct impact to the knee. Medial collateral ligament (MCL) and lateral collateral ligament (LCL) injuries typically result from direct blows to the knee or excessive side-to-side forces. Symptoms of ligament injuries include pain, swelling, instability, difficulty bearing weight, and a popping sensation at the time of injury.
Meniscus Tears: The menisci are C-shaped pieces of cartilage that act as shock absorbers and stabilize the knee joint. Tears in the meniscus commonly occur due to twisting or rotating the knee forcefully, often during sports activities. Symptoms of a meniscus tear include pain, swelling, stiffness, catching or locking sensation in the knee, difficulty fully extending or flexing the knee, and a feeling of instability.
Patellofemoral Pain Syndrome : Patellofemoral Pain Syndrome refers to pain in the front of the knee, specifically around the patella (kneecap). It is often caused by imbalances in the forces acting on the patella, such as weak thigh muscles, overuse, improper alignment of the patella, or abnormal tracking of the patella within the femoral groove. Symptoms include a dull, aching pain in the front of the knee, worsened with activities like climbing stairs, sitting for long periods, or squatting.
Tendinitis: Tendinitis is inflammation of a tendon, commonly caused by repetitive overuse or strain. Patellar tendinitis, also known as jumper’s knee, is a common type of tendinitis affecting the tendon connecting the patella to the shinbone. It often occurs in athletes involved in jumping or running activities. Symptoms include pain, tenderness, and swelling around the patellar tendon, which worsen with activity and improve with rest. Other types of tendinitis that can cause knee pain include quadriceps tendinitis and hamstring tendinitis, which affect the tendons of the thigh muscles.
Signs and Symptoms
Pain: Knee pain can vary in location, severity, and aggravating factors depending on the underlying cause. The pain may be felt in the front of the knee (patellofemoral pain syndrome), behind the knee (Baker’s cyst or tendinitis), on the sides of the knee (lateral or medial collateral ligament injuries), or deep within the joint (osteoarthritis or meniscus tears). The severity of pain can range from mild discomfort to sharp, stabbing pain that limits movement. Aggravating factors may include activities such as walking, running, climbing stairs, squatting, or prolonged sitting or standing.
Swelling: Swelling is a common symptom accompanying knee pain and is often a result of inflammation. Inflammation is the body’s response to injury or irritation and is characterized by increased blood flow to the affected area, resulting in the accumulation of fluid. The knee joint has a synovial lining that produces synovial fluid to lubricate and nourish the joint. When the knee is injured or damaged, the synovial lining may become inflamed, leading to excess synovial fluid production and subsequent swelling. Underlying causes of knee swelling can include injuries such as ligament tears, meniscus tears, bursitis, or conditions like rheumatoid arthritis or gout.
Stiffness: Knee pain often leads to stiffness, which can affect mobility and flexibility. Stiffness is commonly experienced after periods of inactivity, such as waking up in the morning or sitting for an extended time. It can make it difficult to fully bend or straighten the knee joint and may cause a sensation of tightness. Stiffness can be due to inflammation in the joint, which can cause thickening of the synovial lining and limited range of motion. In some cases, the stiffness may also be a result of muscle weakness or tightness around the knee joint.
Instability: Knee instability refers to a feeling that the knee is “giving way” or buckling, making it difficult to bear weight or perform activities with confidence. It can be caused by ligament injuries, such as an anterior cruciate ligament (ACL) tear, which provides stability to the knee joint. When the ligaments are injured, the knee may feel unstable or unreliable during movements that involve changing direction, pivoting, or landing from a jump. Joint laxity, muscle weakness, or damage to other structures like the meniscus can also contribute to feelings of knee instability.
It is important to note that these signs and symptoms can vary depending on the specific cause of knee pain. Consulting with a healthcare professional is recommended for an accurate diagnosis and appropriate treatment.
Diagnostic Tests
When assessing knee pain, healthcare professionals employ a variety of diagnostic tests and procedures to determine the underlying cause. This article provides an overview of common diagnostic methods used in evaluating knee pain, including physical examination, imaging techniques, and arthroscopy.
Physical Examination: A thorough physical examination is often the first step in evaluating knee pain. During this examination, the doctor will assess various aspects, including:
Range of motion: The doctor will evaluate the knee’s ability to bend and straighten fully. Limited range of motion can indicate joint inflammation, cartilage damage, or ligament injuries.
Stability tests: The doctor may perform specific maneuvers, such as the Lachman test or pivot-shift test, to assess the stability of the knee joint. These tests can help identify ligamentous injuries, such as an ACL tear or collateral ligament sprains.
Tenderness: The doctor will palpate the knee to identify areas of tenderness. This helps localize the source of pain and may indicate conditions like patellar tendinitis, bursitis, or osteoarthritis.
Imaging Techniques: Imaging techniques play a crucial role in diagnosing and visualizing internal knee structures. The following imaging modalities are commonly used:
X-rays: X-rays provide a two-dimensional image of the knee joint, allowing visualization of the bones. They can help identify fractures, joint space narrowing (indicative of osteoarthritis), and bone abnormalities. X-rays are readily available, relatively inexpensive, and provide a good initial assessment of bony structures.
Magnetic Resonance Imaging (MRI): MRI utilizes powerful magnets and radio waves to create detailed images of soft tissues, including ligaments, tendons, cartilage, and muscles. It provides excellent visualization of the knee’s internal structures, helping to diagnose ligament tears, meniscus injuries, cartilage damage, and other soft tissue abnormalities.
Computed Tomography (CT) Scan: CT scans use X-ray technology to generate detailed cross-sectional images of the knee joint. While not as commonly used as X-rays or MRI, CT scans may be helpful in assessing complex fractures, identifying bony abnormalities, or when a more detailed evaluation is required.
Arthroscopy: Arthroscopy is a minimally invasive surgical procedure used for both diagnostic and therapeutic purposes. It involves inserting a small camera, called an arthroscope, into the knee joint through a small incision. This allows the doctor to directly visualize the internal structures of the knee, such as the cartilage, ligaments, and synovium. Additionally, surgical instruments can be introduced through additional incisions during the procedure to repair or treat any identified abnormalities. Arthroscopy provides a direct and precise evaluation of the knee joint and is particularly useful for diagnosing and treating conditions like meniscus tears, loose bodies, and certain ligament injuries.
When evaluating knee pain, healthcare professionals utilize a combination of physical examination, imaging techniques (such as X-rays, MRI, and CT scans), and sometimes arthroscopy. These diagnostic procedures aid in identifying the underlying cause of knee pain, guiding appropriate treatment decisions, and facilitating the restoration of optimal knee function. Proper diagnosis is essential for effective management and improved patient outcomes.
Treatment and Management Strategies for Knee Pain
Knee pain is a common complaint among individuals of all ages, affecting their mobility and quality of life. As an orthopedician, I have witnessed numerous cases of knee pain and explored various treatment and management strategies to provide effective relief and improve patient outcomes. There are several approaches for treating knee pain, including both conservative measures and surgical interventions, as well as important management strategies to optimize recovery and prevent future complications.
Initial Assessment and Diagnosis: A thorough evaluation is crucial to accurately diagnose the underlying cause of knee pain. This typically involves a comprehensive medical history review, physical examination, and diagnostic tests such as X-rays, MRI scans, or blood tests. Identifying the root cause enables tailored treatment plans for individual patients.
Treatment and Management Strategies for Knee Pain
Knee pain is a common complaint among individuals of all ages, affecting their mobility and quality of life. As an orthopedic, I have witnessed numerous cases of knee pain and explored various treatment and management strategies to provide effective relief and improve patient outcomes. There are several approaches for treating knee pain, including both conservative measures and surgical interventions, as well as important management strategies to optimize recovery and prevent future complications.
Initial Assessment and Diagnosis
A thorough evaluation is crucial to accurately diagnose the underlying cause of knee pain. This typically involves a comprehensive medical history review, physical examination, and diagnostic tests such as X-rays, MRI scans, or blood tests. Identifying the root cause enables tailored treatment plans for individual patients.
Conservative Treatment Options
Medications: Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, can help reduce pain and inflammation. Topical creams or gels containing analgesics or anti-inflammatory agents may also provide localized relief.
Physical Therapy: Customized exercises and physical therapy programs can strengthen the muscles surrounding the knee, improve flexibility, and promote joint stability. Therapeutic modalities like ultrasound or electrical stimulation may be utilized to aid in pain reduction.
Assistive Devices: The use of assistive devices, such as knee braces, can provide stability, alleviate pressure, and support the knee during daily activities or sports participation.
Weight Management: Maintaining a healthy weight is essential to reduce stress on the knee joint. Weight loss programs and dietary modifications can significantly alleviate knee pain symptoms.
Injections: Corticosteroid Injections: In cases of significant pain and inflammation, corticosteroid injections may be administered directly into the knee joint. These injections can provide temporary relief by reducing inflammation and swelling.
Hyaluronic Acid Injections: Hyaluronic acid injections are designed to lubricate and cushion the knee joint. This treatment option is particularly beneficial for individuals with osteoarthritis-related knee pain.
Surgical Interventions: Arthroscopy: Minimally invasive arthroscopic procedures can be performed to repair or remove damaged structures within the knee joint. This technique allows for faster recovery and minimal scarring.
Partial or Total Knee Replacement: In cases of severe knee pain and functional impairment, partial or total knee replacement surgery may be recommended. This surgical intervention involves replacing the damaged joint surfaces with artificial implants, relieving pain and restoring mobility.
Management and Prevention Strategies:
Rehabilitation: Following any surgical procedure or as part of conservative treatment, a structured rehabilitation program is crucial. It aims to restore strength, flexibility, and range of motion while gradually reintroducing functional activities.
Lifestyle Modifications: Patients should engage in low-impact exercises, such as swimming or cycling, to maintain joint mobility and strength. Avoiding activities that exacerbate knee pain, such as high-impact sports or prolonged kneeling, is also recommended.
Long-Term Monitoring: Regular follow-up appointments with an orthopedician are important to monitor the progress of treatment, address any concerns, and adjust the management plan if necessary.
Injury Prevention: Proactive measures such as wearing appropriate footwear, using proper techniques during physical activities, and implementing warm-up and cool-down exercises can help prevent knee injuries.
Knee pain can significantly impact an individual’s quality of life, but with appropriate treatment and management, relief is possible. A comprehensive approach that combines conservative measures, injections, and surgical interventions tailored to each patient’s specific needs can effectively alleviate pain and restore function. Moreover, implementing lifestyle modifications and preventive strategies can help prevent future knee problems. As an orthopedic, my aim is to provide personalized care and support to patients, guiding them towards optimal knee health and improved overall well-being.